2 Vaccines and Vaccinations: Introduction
Learning Objectives
- Explain the benefits of vaccination on an individual and herd level
- Explain how vaccination confers protective immunity
- Describe types of vaccines and how type alters the animal’s response and vaccination frequency
- Explain why young animals receive a series of vaccinations
- Describe regulatory aspects and to whom one reports vaccine reactions
- Describe risk factors considered when determining a vaccine regimen
- Describe adverse effects of vaccines and vaccination
*
Benefits of Vaccination
The primary benefit of vaccination is the decrease in the number of animals becoming infected with and dying from infections. When many animals are vaccinated, this “herd effect” has benefit for the vaccinated animals, which are unlikely to become ill from a disease for which they have been vaccinated, and for all animals in the population, who are less likely to be exposed to the disease. This also has public health significance; rabies would be a significant threat to human health in the United States without vaccination of domestic animals.
Objectives of Vaccination
- To vaccinate the largest possible number of individuals in the population at risk
- To vaccinate each individual no more frequently than necessary
- To vaccinate only against agents to which the animal has a realistic risk of exposure and subsequent development of serious disease
*
Vaccination Confers Protective Immunity
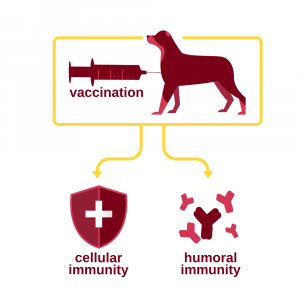
Vaccination is controlled exposure of an animal’s immune system to something that causes disease. Vaccination is the act; immunization is the desired result. In veterinary medicine, most vaccines are developed against viruses; some protect against specific bacteria or toxins. When an animal is vaccinated, its immune system recognizes the foreign proteins and builds up a response to them. Part of that response is the creation of antibodies, proteins that bind to the pathogen and lead to its destruction (humoral immunity). This is moderated through immune cells in the lymphatic system including B Cells and T cells that process the vaccine components. At a superficial level, B cells produce antibodies based on the vaccine components, which then circulate and label pathogens. This allows T cells to identify and attack pathogens tagged by antibodies as well as signal the immune system.
Another part of that response is creation of cells within the animal’s body that will destroy that pathogen (cellular immunity). Some of those cells are memory cells and are capable of generating a faster and stronger response every time the animal is re-exposed to the pathogen. This means that vaccinated animals, which have created a store of memory cells, can respond quickly to any natural exposure to the pathogen and are significantly less likely to become ill.

*
Types of Vaccines
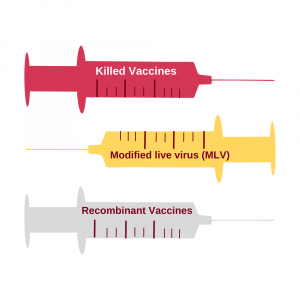
There are three types of vaccines available for use by veterinarians.
1. Killed vaccines (also called inactivated vaccines) contain inactivated whole viruses or bacteria. Killed vaccines are more stable for handling and storage and are incapable of causing disease in the animal but require use of an adjuvant, which may be associated with vaccine reactions. Killed vaccines may not generate a long-lasting immune response, often requiring them to be given more frequently to be effective. The first time a killed vaccine is given, it primes the immune system but does not evoke an immune response; the animal must get a booster or be naturally exposed for an immune response to occur.
2. Modified live virus (MLV) vaccines (also called attenuated vaccines) contain whole viruses that are not dead but are treated such that they can no longer cause disease. Because the organism in the MLV vaccine is alive and can replicate, these may occasionally cause diseases in vaccinated animals. These vaccines generally stimulate a much stronger and long-lived immune response. Because these may occasionally cause disease in vaccinated animals, their use must be timed carefully; for example, many MLV vaccines cannot be given to pregnant animals as they may cause abortion. Caution also must be used in giving these vaccines to immunosuppressed animals.
3. Recombinant or subunit vaccines use portions of viruses or bacteria to generate an immune response. These cannot cause disease in vaccinated animals but do not always generate an adequate immune response. Recombinant technology is improving steadily and it is anticipated that in the future, recombinant vaccines could be the preferred type. Because an animal’s response to vaccination is not dependent on “dose” of vaccine provided, the same amount of vaccine is given to all animals in a given species.
*
Vaccination Series
The earliest age at which vaccines can be given and the need for boostering is defined by the manufacturer. Young animals that nursed from their dam within the first day of life will have antibodies from her first milk (colostrum) that were taken up across their GI tract into their general circulation (passive immunity). Those antibodies will interfere with vaccines and often we do not know when those antibody concentrations decline. Young animals also are variable in timing of function of their own immune function (active immunity). Because of this, young animals often receive a series of vaccines, with timing of boosters defined by the manufacturer. In adult animals, some vaccines are boostered when first given and others are not; directions for use on the vaccine label always should be followed.
The goal of boostering vaccines in adult animals is to create an elevation in immune response to protect against disease challenge. Timing of boosters is dependent on the type of vaccine used (killed versus MLV, for example) and on the characteristics of the organism itself. The manufacturer provides guidelines for optimal intervals for boostering of vaccine. What if the animal (young or adult) is overdue for vaccines? There are various conversations evaluating immune response in animals vaccinated with an inappropriately long boostering interval. Veterinarians must use their common sense and knowledge of immunology (or in the case of rabies, they must follow the law). Guidelines are available from the American Animal Hospital Association and American Association of Feline Practitioners to answer this concern for dogs and cats.
*
Regulatory Aspects of Vaccination
There is a lot of controversy regarding how many antigens one should include at one time for vaccination against disease. Some argue that the immune system has built-in systems to be duplicative, so even if only a couple of B cells respond to a given antigen, that will trigger production of more B cells and a quick amplification of antibody concentrations. Others argue that the body can only respond to so many attacks at one time because there are a finite number of B cells and T cells available as antigens are introduced, so the animal (or person) either won’t respond to some of the antigens or will do so improperly. Those who argue this latter point often make the jump that what we are doing is inducing an abnormal immune response, and autoimmune disease, where antibodies or T cells are triggered to destroy host tissue. None of this is particularly well evaluated using the scientific method. A non-medical piece to the puzzle is client compliance; if you get one chance to vaccinate that animal, is it wisest to vaccinate against all diseases of concern, recognizing that the client may not return with that animal for further vaccines if you choose to limit what you offer at a given time?
All vaccines used by veterinarians must be approved by the United States Department of Agriculture (USDA) and demonstrated to be pure, safe, potent, and effective. It is from this USDA approval process that the manufacturer determines what information will be on the vaccine label. The USDA considers a vaccine safe if it does not cause “undue local or systemic responses.” After the vaccine is licensed and marketed, no continuing measurement of risk is required. An adverse reaction is defined by the USDA as “any undesirable side effect or unintended effect (including lack of desired result) associated with the administration of a licensed biological product”. All adverse reactions reported by veterinarians to the manufacturer are reported to the USDA and if you wish, you may contact the USDA directly. If veterinarians do not report adverse effects, the manufacturer may not be aware they are occurring. Here is information from Dr. Richard Ford: “In veterinary medicine, there is no mandate to report a vaccine adverse reaction, whether the reaction is known to have been caused by a vaccine or merely suspected to have been. Although encouraged to do so, formal reports from the veterinarians to the USDA are seldom filed. Veterinarians who do report known or suspected reactions tend to contact the manufacturer directly. However, neither the licensing agencies nor the vaccine manufacturers are under obligation to provide a veterinarian with additional information regarding either the number of type of vaccine adverse events. Today, there are no data available to veterinarians that specifically address surveillance or documentation of vaccine adverse reactions in companion animals. Manufacturers are under no obligation to compensate the owner or the veterinarian for diagnostic or treatment services related to a known or suspected adverse event.”
True effectiveness of a vaccine often is unknown. Challenge testing, in which unvaccinated and vaccinated animals are exposed to the virus and the number that become ill compared, is not always performed. Duration of immunity (the amount of time an animal is protected from disease after vaccination) is not known for all vaccines approved by the USDA, and can vary widely amongst individuals.
*
Risk Factors of Vaccinations
Risk factors to be considered include host factors specific to that animal, environmental factors, and agent factors specific to that vaccine. Animals that are malnourished, are ill with another disease or condition, or are stressed are unlikely to respond well to vaccination. Young animals (for example, puppies and kittens less than 16 weeks of age) may still have significant levels of antibodies from their mother, taken in when they nursed in their first day of life. These antibodies may inactivate the vaccine, rendering it useless. Environmental factors look at the population as a whole. The more animals there are in the population, the greater the likelihood any one animal will be exposed to a given virus. Those animals that are exposed to new animals, for example by introduction of a new pet, or by boarding or grooming, are at greater risk. The final thing to assess is the virus and disease itself. Rabies is an example of a virus that kills all the dogs and cats it infects and can kill exposed humans if they are not treated promptly. Any risk of vaccination is outweighed by the huge risk of death if infected with the virus.
Examples of Risk Factors of a Vaccine Regimen for Horses
- Risk of infection and disease (geography, horse age, occupation, movement patterns)
- Medical, economic, and logistic consequences of disease should it occur
- Potential for spread of infection to other horses and/or humans
- Farm size and type
- Vaccine cost, availability, and efficacy
- Risk of adverse reactions to vaccination
*
Diseases occur due to multiple factors. Their relationship is sometimes called the infection triangle.All three factors (environment (e.g. management practices), host, and pathogen) are important for the development or prevention of disease and all three need to be considered during disease prevention.
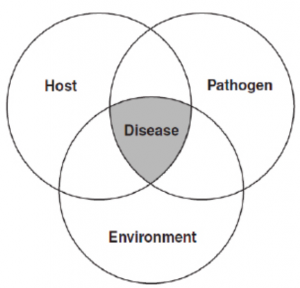
—
*
Adverse Effects of Vaccination
Adverse effects of vaccination have been attributed to preservatives in the vaccine, contaminants, the organism itself, products added to enhance the immune response (adjuvants), and to the administration of multiple vaccines at one time. In most cases, neither the cause nor the exact likelihood of an adverse effect is known.
There are two main types of vaccine reactions, systemic and local. Systemic reactions occur throughout the body, not just at the site of administration of the vaccine, and usually are non-specific. Examples include lack of appetite, fever and soreness. Allergic reactions may occur. These may be sudden, with onset immediately after vaccination and clinical signs lasting for up to two days. Signs of an allergic reaction include swelling of the face and respiratory distress. Some advocate giving less vaccine to minimize allergic reactions but since neither allergic reactions nor immunization are “dose” dependent, there is little wisdom in this practice. Autoimmune diseases are those conditions in which the immune system of an animal or person starts to destroy that individual’s normal tissue. While people have hypothesized that autoimmune disease could be induced by vaccination, there is little scientific evidence of such a connection.
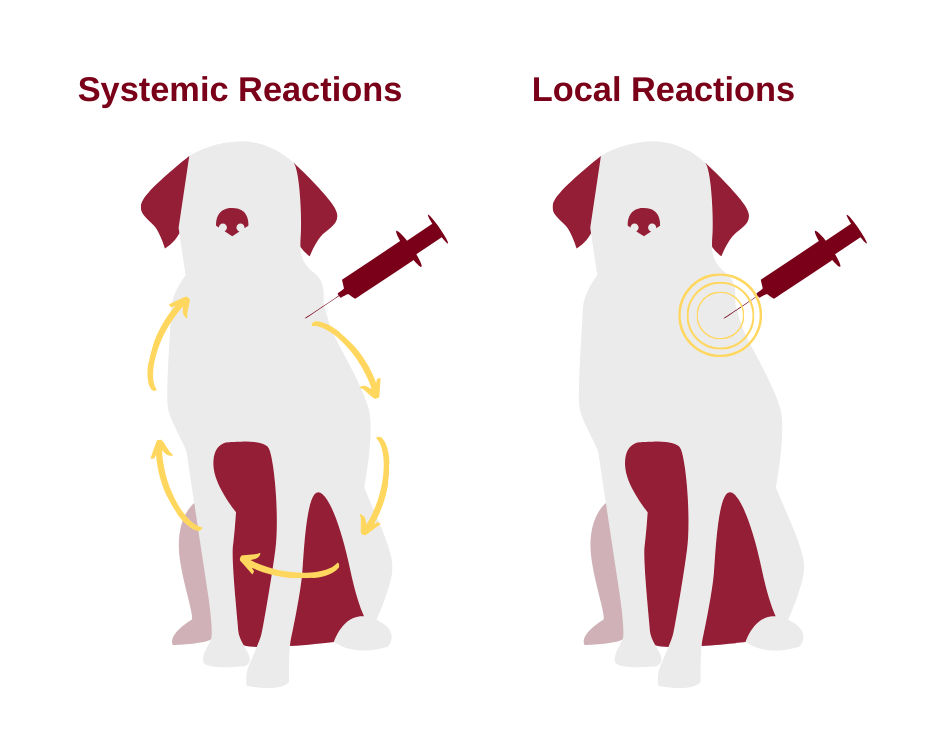
Local adverse vaccine reactions include pain at the injection site, hair loss or change in hair color at the injection site, and swellings. Swellings that develop fairly soon after the vaccination, are non-painful, and feel soft usually are benign sites of inflammation. They resolve over weeks to months. Pain may develop if the vaccine is inadvertently administered near a nerve. Some vaccines cause more pain than others when administered because of their chemical composition.
A final possible adverse effect of a vaccine is vaccine virulence, in which the vaccine causes the disease it was designed to protect against. This can only occur with modified live vaccines, which contain the whole virus. Likelihood of this occurring is very dependent on the host into which the vaccine is being injected. For example, a vaccine that is safe for adult animals may cause disease in very young animals. Some modified live vaccines can induce birth defects if given to pregnant animals. Vaccines are more likely to become virulent if used in the wrong species (for example, using an unapproved feline vaccine in ferrets) or if given by the wrong route (for example, cats that lick at the injection site may take some vaccine in by mouth, with a return to virulence when the vaccine contacts the mucous membranes of their gums).
Vaccines are designated as core or non-core (risk-based). Core vaccines are those that are recommended for administration to every animal, based on (1) universal susceptibility to disease caused by a specific infectious organism; (2) significant risk that animals in the area will become infected; (3) likelihood of significant medical consequences to the animal as a result of infection and disease; (4) availability of a vaccine that is both safe and highly effective; and (5) possible risk of zoonosis. In other words, core vaccines are those for infectious diseases for which the benefit-risk-cost relationship is clear for all animals and the decision to vaccinate is straightforward. Non-core, or risk-based, vaccines are recommended only when an animal’s lifestyle is such that they are at increased risk of exposure to the disease. These diseases usually will resolve spontaneously or respond readily to treatment. One method of determining whether or not a vaccine should be given to a specific animal is to use some sort of scoring rubric such as that below.

*
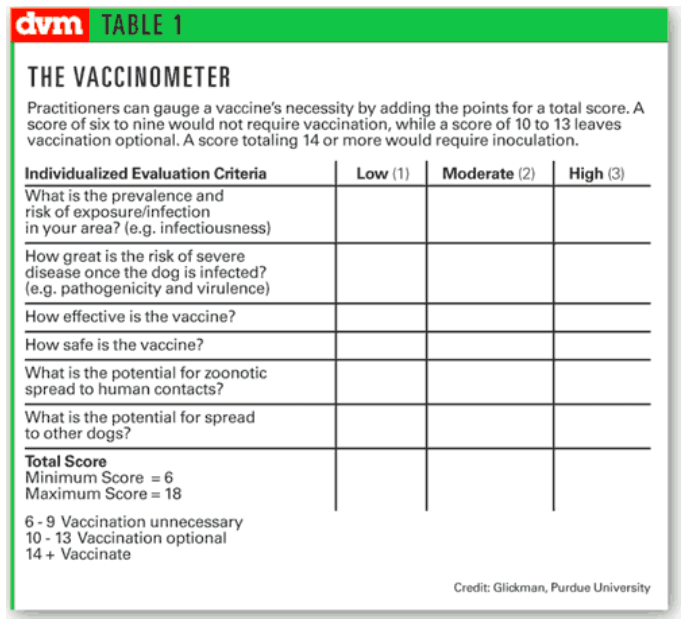
*
 Extra resources
Extra resources
- AVMA Vaccination principles: https://www.avma.org/KB/Policies/Pages/Vaccination-Principles.aspx


